How Many Days After a Tb Test Should It Be Read
| Mantoux test | |
|---|---|
 The Mantoux skin test consists of an intradermal injection of one-tenth of a milliliter (ml) of PPD tuberculin. The circular shape is known every bit a wheal response. | |
| Synonyms | Mantoux screening test |
| Purpose | screen for tuberculosis |
The Mantoux test or Mendel–Mantoux test (also known as the Mantoux screening examination, tuberculin sensitivity test, Pirquet test, or PPD test for purified protein derivative) is a tool for screening for tuberculosis (TB) and for tuberculosis diagnosis. Information technology is one of the major tuberculin skin tests used effectually the world, largely replacing multiple-puncture tests such as the tine test. The Heaf exam, a grade of tine test, was used until 2005 in the U.k., when information technology was replaced by the Mantoux test. The Mantoux test is endorsed by the American Thoracic Guild and Centers for Disease Control and Prevention. It was also used in the USSR and is now prevalent in well-nigh of the mail-Soviet states.
History [edit]
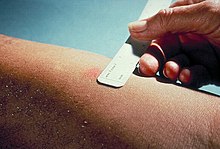
The size of induration is measured 48–72 hours later. Erythema (redness) should non be measured.

Mantoux exam injection site in a subject area without chronic conditions or in a high-risk group clinically diagnosed as negative at 50 hours
Tuberculin is a glycerol extract of the tubercle bacillus. Purified protein derivative (PPD) tuberculin is a precipitate of species-nonspecific molecules obtained from filtrates of sterilized, full-bodied cultures. The tuberculin reaction was first described by Robert Koch in 1890. The examination was beginning developed and described by the German doc Felix Mendel in 1908.[1] Information technology is named after Charles Mantoux, a French physician who built on the piece of work of Koch and Clemens von Pirquet to create his exam in 1907. However, the test was unreliable due to impurities in tuberculin which tended to cause false results.[2]
Esmond R. Long and Florence B. Seibert identified the active agent in tuberculin as a protein. Seibert then spent a number of years developing methods for separating and purifying the protein from Mycobacterium tuberculosis, obtaining purified protein derivative (PPD) and enabling the creation of a reliable test for tuberculosis.[2] Her first publication on the purification of tuberculin appeared in 1934.[3] By the 1940s, Seibert's PPD was the international standard for tuberculin tests.[iv] In 1939, M. A. Linnikova in the USSR created a modified version of PPD. In 1954, the Soviet Matrimony started mass production of PPD-L, named after Linnikova.[5] [half-dozen]
Procedure [edit]
In the Mantoux test, a standard dose of 5 tuberculin units (TU - 0.1 ml), according to the CDC,[7] or 2 TU of Statens Serum Institute (SSI) tuberculin RT23 in 0.1 ml solution, co-ordinate to the National Health Service,[8] is injected intradermally (between the layers of dermis) on the flexor surface of the left forearm, mid-style betwixt elbow and wrist. The injection should be made with a tuberculin syringe, with the needle bevel facing upward. Alternatively, the probe can be administered by a needle-gratis jet injector. When placed correctly, injection should produce a pale wheal of the pare, 6 to 10 mm in diameter. The result of the examination is read subsequently 48–96 hours merely 72 hours (third day) is the ideal. This intradermal injection is termed the Mantoux technique. A person who has been exposed to the leaner is expected to mount an immune response in the skin containing the bacterial proteins. The response is a classical example of delayed-type hypersensitivity reaction (DTH), a type Iv of hypersensitivities. T cells and myeloid cells are attracted to the site of reaction in the timeframe of i–3 days and generate local inflammation. The reaction is read by measuring the diameter of induration (palpable raised, hardened surface area) beyond the forearm (perpendicular to the long axis) in millimeters. If at that place is no induration, the result should be recorded as "0 mm". Erythema (redness) should not be measured.[ citation needed ] In the Pirquet version of the test tuberculin is applied to the skin via scarification.[ix]
Nomenclature of tuberculin reaction [edit]
The results of this test must exist interpreted carefully. The person's medical risk factors determine at which increment (5 mm, 10 mm, or fifteen mm) of induration the upshot is considered positive.[x] A positive outcome indicates TB exposure.
- 5 mm or more than is positive in
- An HIV-positive person
- Persons with recent contacts with a TB patient
- Persons with nodular or fibrotic changes on chest X-ray consistent with sometime healed TB
- Patients with organ transplants, and other immunosuppressed patients
- 10 mm or more is positive in
- Recent arrivals (less than five years) from high-prevalence countries
- Injection drug users
- Residents and employees of high-risk besiege settings (due east.yard., prisons, nursing homes, hospitals, homeless shelters, etc.)
- Mycobacteriology lab personnel
- Persons with clinical atmospheric condition that place them at high hazard (e.g., diabetes, prolonged corticosteroid therapy, leukemia, terminate-stage renal disease, chronic malabsorption syndromes, depression body weight, etc.)
- Children less than 4 years of historic period, or children and adolescents exposed to adults in high-run a risk categories
- 15 mm or more is positive in
- Persons with no known risk factors for TB[11]
A tuberculin test conversion is defined as an increment of ten mm or more within a two-year flow, regardless of age. Alternative criteria include increases of 6, 12, 15 or 18 mm.[12]
False positive result [edit]
TST (tuberculin skin test) positive is measured by size of induration. The size of the induration considered to be a positive effect depends on run a risk factors. For example, a depression-risk patient must have a larger induration for a positive issue than a high-hazard patient. High-risk groups include recent contacts, those with HIV, those with chest radiograph with fibrotic changes, organ transplant recipients, and those with immunosuppression.
According to the Ohio Department of Wellness and US Department of Health, the Bacillus Calmette–Guérin (BCG) vaccine does not protect against TB infection. It does, though, give 80% of children protection confronting tuberculous meningitis and miliary tuberculosis. Therefore, a positive TST/PPD in a person who has received BCG vaccine is interpreted every bit latent TB infection (LTBI).[13] Due to the exam'due south depression specificity, most positive reactions in depression-take chances individuals are false positives.[fourteen] A fake positive issue may be caused past nontuberculous mycobacteria or previous administration of BCG vaccine. Vaccination with BCG may outcome in a false-positive result for many years after vaccination.[15]
False positives can also occur when the injected expanse is touched, causing swelling and itching. If the swelling is less than five mm, information technology is possibly due to error past the healthcare personnel causing inflammation to the area.
Another source of false positive results can be allergic reaction or hypersensitivity. Although rare, (about 0.08 reported reactions per million doses of tuberculin), these reactions can be dangerous and precautions should be taken past having epinephrin available.[16]
False negative outcome [edit]
Reaction to the PPD or tuberculin test is suppressed by the following conditions:
- Recent TB infection (less than eight–10 weeks)
- Infectious mononucleosis
- Live virus vaccine - The test should non be carried out within 3 weeks of live virus vaccination (due east. thousand. MMR vaccine or Sabin vaccine).
- Sarcoidosis
- Hodgkin's illness
- Corticosteroid therapy/steroid use
- Malnutrition
- Immunological compromise - Those on immuno-suppressive treatment or those with HIV and low CD4 T cell counts, oftentimes testify negative results from the PPD test.[ citation needed ]
This is because the allowed system needs to be functional to mount a response to the poly peptide derivative injected under the skin. A simulated negative result may occur in a person who has been recently infected with TB, merely whose immune system hasn't yet reacted to the bacteria.
- Upper respiratory virus infection
In case a 2d tuberculin exam is necessary it should be carried out in the other arm to avoid hypersensitising the skin.
BCG vaccine and the Mantoux test [edit]
The part of Mantoux testing in people who have been vaccinated is disputed. The US recommends that tuberculin skin testing is non contraindicated for BCG-vaccinated persons, and prior BCG vaccination should not influence the interpretation of the exam. The UK recommends that interferon-γ testing should be used to help interpret positive Mantoux tests of over 5mm,[17] and repeated tuberculin skin testing must non be done in people who have had BCG vaccinations. In general, the United states recommendation may result in a larger number of people beingness falsely diagnosed with latent tuberculosis, while the UK approach has an increased take a chance of missing patients with latent tuberculosis who should be treated.[ citation needed ]
According to the US guidelines, latent tuberculosis infection diagnosis and handling is considered for any BCG-vaccinated person whose peel test is x mm or greater, if any of these circumstances are present:
- Was in contact with another person with infectious TB
- Was born or has lived in a high TB prevalence country
- Is continually exposed to populations where TB prevalence is high
Anergy testing [edit]
In cases of anergy, a lack of reaction past the torso's defense mechanisms when information technology comes into contact with foreign substances, the tuberculin reaction will occur weakly, thus compromising the value of Mantoux testing. For example, anergy is present in AIDS, a disease which strongly depresses the allowed system. Therefore, anergy testing is advised in cases where at that place is suspicion that anergy is present. However, routine anergy skin testing is not recommended.[xviii]
Two-step testing [edit]
Some people who have been infected with TB may have a negative reaction when tested years after infection, every bit the immune organization response may gradually wane. This initial skin test, though negative, may stimulate (boost) the torso'south ability to react to tuberculin in future tests. Thus, a positive reaction to a subsequent test may be misinterpreted equally a new infection, when in fact it is the event of the boosted reaction to an old infection.[nineteen]
Utilise of two-step testing is recommended for initial pare testing of adults who will exist retested periodically (due east.g., wellness intendance workers). This ensures any future positive tests can be interpreted as being acquired past a new infection, rather than only a reaction to an erstwhile infection.
- The first exam is read 48–72 hours afterwards injection.
- If the commencement exam is positive, consider the person infected.
- If the first test is negative, give a 2nd test ane to three weeks afterward the commencement injection.
- The second exam is read 48–72 hours subsequently injection.
- If the second exam is positive, consider the person infected in the afar past [20]
- If the second examination is negative, consider the person uninfected.[21]
A person who is diagnosed as "infected in the afar past" on two-step testing is chosen a "tuberculin reactor".
The United states of america recommendation that prior BCG vaccination exist ignored results in almost universal simulated diagnosis of tuberculosis infection in people who have had BCG (mostly strange nationals).
The latest estimation for Mantoux examination results [edit]
According to the guidelines published by Centers for Disease Command and Prevention in 2005, the results are re-categorized into iii parts based on their previous or baseline outcomes:
- Baseline test: ≥10 mm is positive (either first or 2d step); 0 to nine mm is negative
- Series testing without known exposure: Increment of ≥10 mm is positive
- Known exposure:
- ≥5 mm is positive in patients with baseline of 0 mm
- ≥10 mm is positive in patients with negative baseline or previous screening outcome of >0 mm
Contempo developments [edit]
In addition to tuberculin peel tests such as (principally) the Mantoux test, interferon gamma release assays (IGRAs) accept become common in clinical use in the 2010s. In some contexts they are used instead of TSTs, whereas in other contexts TSTs and IGRAs both continue to be useful.[22]
The QuantiFERON-TB Gold blood test measures the patient's immune reactivity to the TB bacterium, and is useful for initial and series testing of persons with an increased risk of latent or active tuberculosis infection. Guidelines for its use were released past the CDC in Dec 2005.[23] QuantiFERON-TB Gilt is FDA-approved in the United States, has CE Marking approval in Europe and has been canonical by the MHLW in Japan. The interferon gamma release analysis is the preferred method for patients who take had immunosuppression and are near to starting time biological therapies.[24]
T-SPOT.TB is some other IGRA; information technology uses the ELISPOT method.
Heaf test [edit]
The Heaf tuberculin skin exam was used in the United kingdom of great britain and northern ireland, but discontinued in 2005. The equivalent Mantoux test positive levels washed with ten TU (0.1 ml at 100 TU/ml, one:1000) are[ citation needed ]
- <five mm induration (Heaf 0–one)
- v–fifteen mm induration (Heaf ii)
- >fifteen mm induration (Heaf 3–4)
Run across also [edit]
- Tuberculosis
- Latent tuberculosis
- QuantiFERON
- Tine examination
References [edit]
- ^ F. Mendel. Therapeutische Monatshefte, Berlin, 1903, 16: 177. Die von Pirquet'sche Hautreaktion und die intravenöse Tuberkulinbehandlung.Medizinische Klinik, München, 1908, four: 402-404.
- ^ a b "Esmond R. Long and Florence B. Seibert". Chemic Heritage Foundation. Archived from the original on January 13, 2012. Retrieved April 27, 2011.
- ^ "Florence Seibert, American Biochemist, 1897–1991". Chemistry Explained . Retrieved 26 October 2015.
- ^ Dacso, C. C. (1990). "Chapter 47: Skin Testing for Tuberculosis". In Walker, H. K.; Hall, Due west. D.; Hurst, J.W. (eds.). Clinical Methods: The History, Physical, and Laboratory Examinations (3rd ed.). Boston: Butterworths. ISBN9780409900774 . Retrieved 26 Oct 2015.
- ^ "Mantoux examination,Mantoux test inventors". Edubilla.com . Retrieved 2019-04-25 .
- ^ "Mantoux test | Clinical Medicine | Medical Specialties". Scribd . Retrieved 2019-04-25 .
- ^ "TB Elimination - Tuberculin Skin Testing" (PDF). CDC.gov. CDC - National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention - Sectionalisation of Tuberculosis Elimination. Oct 2011. Retrieved 5 June 2017.
- ^ "The Mantoux test: Administration, reading and estimation" (PDF). NHS.united kingdom. Archived from the original (PDF) on 15 Feb 2010. Retrieved five June 2017.
- ^ "Pirquet's skin exam | medicine".
- ^ From the CDC squad of the CDC team at the Saskatchewan Lung Association, photos of a PPD crash-land Archived 2007-03-21 at the Wayback Machine.
- ^ Mantoux Test Archived 2016-09-xxx at the Wayback Machine in eac.int.
- ^ Menzies, Dick (one January 1999). "Estimation aof Repeated Tuberculin Tests". American Journal of Respiratory and Disquisitional Intendance Medicine. 159 (one): 15–21. doi:10.1164/ajrccm.159.ane.9801120. PMID 9872812.
- ^ Data also from ODH lecture at the Ohio Land University five/24/2012.
- ^ Starke JR (Jul 1996). "Tuberculosis Skin Testing: New Schools of Thought". Pediatrics. 98 (i): 123–125. doi:10.1542/peds.98.i.123. ISSN 0031-4005. PMID 8668383. S2CID 19907614.
- ^ Chaturvedi N, Cockcroft A (1992). "Tuberculosis screening among health service employees: who needs breast X-rays?". J Soc Occup Med. 42 (iv): 179–82. doi:ten.1093/occmed/42.4.179. PMID 1421331.
- ^ James E. Froeschle; Frederick Fifty. Ruben; A. Michael Bloh (2002). "Immediate Hypersensitivity Reactions afterwards Employ of Tuberculin Skin Testing". Clinical Infectious Diseases. 34 (one): e12–e13. doi:10.1086/324587. PMID 11731966.
- ^ "Recommendations | Tuberculosis | Guidance | NICE".
- ^ Markowitz, Norman (1993). "Tuberculin and Anergy Testing in HIV-Seropositive and HIV-Seronegative Persons". Ann Intern Med. 119 (3): 185–193. doi:10.7326/0003-4819-119-3-199308010-00002. PMID 8100692. S2CID 37590470.
- ^ "Fact Sheets | Testing & Diagnosis | Fact Sail - Tuberculin Pare Testing | TB | CDC". www.cdc.gov. 2018-12-11. Retrieved 2019-05-29 .
- ^ "Information on Ii-Step TB Skin Test" (PDF). Archived from the original (PDF) on 2020-08-03. Retrieved 2017-03-13 .
- ^ Role of Health and Human Services. "Booster Phenomenon". Retrieved 2008-07-02 .
- ^ Collins, LF; Geadas, C; Ellner, JJ (2016), "Diagnosis of latent tuberculosis infection: too soon to pull the plug on the tuberculin skin examination", Ann Intern Med, 164 (ii): 122–124, doi:10.7326/M15-1522, PMID 26642354, S2CID 1059756.
- ^ Guidelines for Using the QuantiFERON-TB Gold Test for Detecting Mycobacterium tuberculosis Infection, United States
- ^ British Association of Dermatologists guidelines for biologic therapy for psoriasis 2017* www.bad.org.uk, accessed xi October 2020
Source: https://en.wikipedia.org/wiki/Mantoux_test
0 Response to "How Many Days After a Tb Test Should It Be Read"
Enviar um comentário